Langerhans cell Histiocytosis (LCH)
Description:
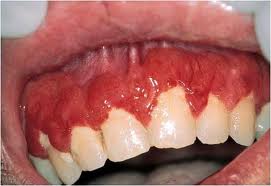
Langerhans Cell Histiocytosis is a disease that involves abnormal proliferation of cells known as the Langerhans cells which is a type of white blood cell that the body produces to help fight infection. These cells come from our bone marrow, lungs, and skin and migrate to the lymph nodes. This condition occurs when the body produces too many of these cells. LCH can occur in anyone, but is most common in children. Oral changes such as gingival ulcerations, osseous lesions associated with tooth mobility, and early loss of primary teeth are common.
Diagnostic Factors:
In the article I chose to discuss, a mother had brought in her child whose chief complaint was bleed gums, and mobile teeth. The dental team had to do a biopsy of the tissue to diagnose what the problem was. Diagnosis of this disease is confirmed through biopsy and routine tests as well, such as blood count and liver function. Radiographs are also helpful in the determination of the extent of the damage to the bone and lungs.
Etiology and Prevalence:
Pathogens and Etiology are unknown, however, LCH is a rare disorder with an incidence of 5:1,000,000. More then 50% of all cases involve children younger than fifteen, with a peak in children 1-4 and affects more males then females. LCH commonly affects the head and neck region, particularly skull bones, including the maxilla and mandible. LCH disease has three different clinical forms they are as followes:
Letterer-Siwe Diseas
Acute, fulminant, proliferative form, mostly new-born babies, and children younger than 3 years old disseminated osseous, visceral, and skin involvement.
Hand-Schüler-Christian
Disease disseminated, chronic form classic triad: multiple bone lesions of the skull Exophthalmos Diabetes insipidus mostly children older than 3 years old and young adults
Eosinophilic granuloma
Chronic, localized form solitary or multiple skeletal lesions no visceral or skin involvement more frequent in children and young adults
Patient Education:
To educate the patient you should first have them diagnosed. Then once diagnosed they can be treated. LCH can be confused with other disease such as, diabetes-associated periodontitis, hypophosphateasia, leukemia cyclic neutropenia, fibrous dysplasia, Papillon-Lefèvre disease, agranulocytosis, and malignant neoplasm’s. Therefore, it is important to make sure the patient has the right information on the disease.
Treatment:
Due to the heterogeneity involving this pathology, there is no consensus about which is the best treatment. Surgical removal is the treatment of choice for single osseous lesions, whereas lesions difficult to access or involving multiple organs are treated with radiotherapy or chemotherapy. Dental intervention should not include extraction of all teeth involved, but only those having either severe mobility or lytic bone lesions associated with the root apex. Therefore, extractions combined with chemotherapy provided intra/extra-oral regression of this patient’s symptoms.
AAP:
Guimarães, L., Dias, P., Janini, M., & de Souza,
I. (2008). Langerhans cell histiocytosis: impact on the permanent dentition
after an 8-year follow-up. Journal Of Dentistry For Children (Chicago,
Ill.), 75(1), 64-68.